Common Pains. Common Procedure. There’s a Connection.
Three clients in two days. Three different pain profiles.
Each day at the Bridging Institute we see a variety of people with pain and movement concerns. Recently I met three people in two days with mystery pains. At first glance, the pain issues from all three clients seemed unrelated. But there ended up being a common thread.
The three challenges included:
- Back pain when lifting medium weight things at work
- Hip pain when walking
- Back spasms after yoga
The common thread? They each had a minimally invasive surgical procedure in their past. The movement disruption from the procedure factored into the structural stress, which resulted in pain.
In this series, we’ll explore why one of the most common types of surgical procedures can create long-lasting stress in the body — often showing up as pain months or even years later.
What we’ll cover over the coming weeks
- Week 1: The procedure—and why it disrupts movement
- Week 2: Bridging® support at different points in the recovery process
- Week 3: Why the support for children vs. adults differs
- Week 4: What you can do to help yourself
Minimally Invasive Surgery … With Lasting Effects
 Each of these clients had one thing in common: a history of laparoscopic surgery. The timing varied — weeks ago, months ago, even years ago. Why is this such a common root cause?
Each of these clients had one thing in common: a history of laparoscopic surgery. The timing varied — weeks ago, months ago, even years ago. Why is this such a common root cause?
In case you’re not familiar with this type of surgery, these are the most common reasons the process is used:
- Appendix removal
- Gallbladder removal
- Hernia repair
- Gynecological procedures
- Colon resections
Yes — laparoscopic surgery is a game changer. These are the reasons this approach has become so widely used:
- Faster recovery
- Lower infection risk
- Shorter healing window (often around 6 weeks)
If you are like most of the clients we meet who have had these types of surgery, you’ll recognize the following about the procedure:
- You have a few small scars
- They placed tubes for the procedure via the scar locations
- Once healed, you were cleared to return to activity
And that’s usually where the interaction with your medical team ends.
But here’s what often gets missed … being “healed” does not mean your body’s ability to move has fully recovered.
Generally, medical follow-up does not assess:
- How your muscles are coordinating
- Whether your core muscles are functioning as they should
- How your movement patterns may have changed
And yet — these movement changes are very real, and don’t usually resolve with time.
What Actually Happens During the Procedure
To understand why movement is affected, it helps to understand a few parts of the process used.
There are three key parts of the laparoscopic surgery process, and often clients are unaware of the first part of the procedure — expanding the abdomen like a balloon with gas.
Here are more details about the overall process and why each part can create challenges.
 1. Abdominal Distension (Gas Inflation)
1. Abdominal Distension (Gas Inflation)
Carbon dioxide is used to expand the abdominal cavity, creating space for the procedure.
This alters:
- How the abdominal muscles relate to each other
- How the core connects with the back muscles
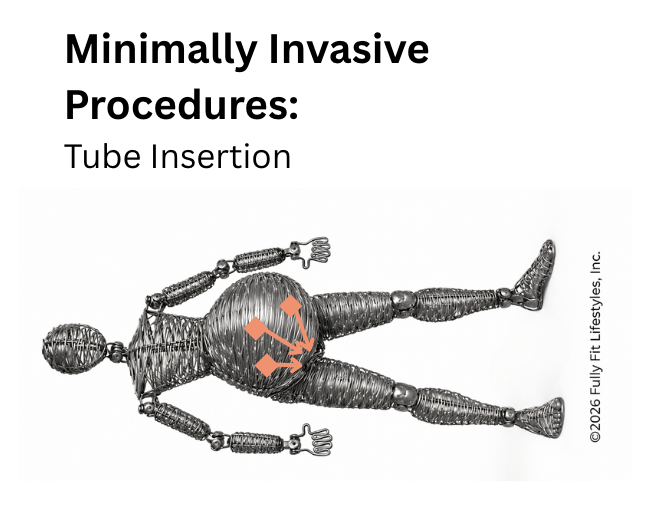
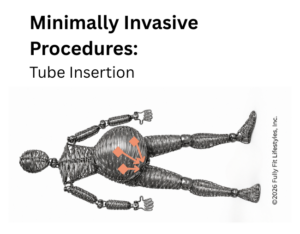 2. Tube Insertion
2. Tube Insertion
Surgical tools are inserted via tubes through the abdominal wall. The entry scars are often near the belly button and a few inches to the side.
This process:
- Pushes through multiple layers of muscle and tissue
- Can shift how those muscle layers coordinate
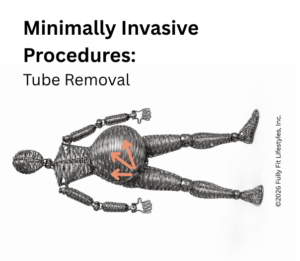 3. Tube Removal
3. Tube Removal
When the instrument tubes are removed, the abdominal tissue is again stressed and irritated.
This can further:
- Disrupt muscle coordination by ‘dragging’ tissue directionally
- Leave space in the wake of tube removal allowing abdominal tissue to settle in a different orientation which impacts muscle coordination
Why This Disruption Matters
Each body responds differently — but the pattern of disruption is remarkably consistent. That’s why we specifically ask about laparoscopic procedures on our intake forms — and test how the noted characteristics may be contributing to current pain or movement limitations.
Common pain patterns observed
Because the abdomen plays such a central role, the effects often show up in predictable ways:
- Abdominal discomfort that is present when active
- Low back pain
- Hip pain
- Limited hip mobility or tightness
- Sensation of core weakness
These aren’t random. They’re structural shifts in the body from the procedure’s process.